In most countries, health improved dramatically during the twentieth century, with large increases in life expectancy. In the United Kingdom (UK), life expectancy at birth has increased by more than half. According to recent estimates, it nearly doubled in other high-income countries (1, 2) and is anticipated to continue to climb (3). The tremendous growth in life expectancy among generations has prompted the question of how the extra years of life would be spent healthily.
Lifestyle changes and medical breakthroughs may be able to provide us an extra six years of quality life. Life expectancy at birth in America was 35 years in 1800, then it gradually increased to 39.4 years in 1880, then to 78.9 years in 2019 (4).
Although increased life expectancy is rarely viewed as a negative, what if those extra years are spent in poor health?
According to a new analysis from the McKinsey Health Institute, we are currently spending more years in poor health than at any other period in history (MHI).
According to a growing but fragmented body of evidence, those born after 1945 have had increasingly worse health at the same age in other areas. This has been shown for subjective health metrics like self-reported health (5) and disability such as self-reported health conditions such as diabetes, high blood pressure, and mental health disorders (6).
Global differences
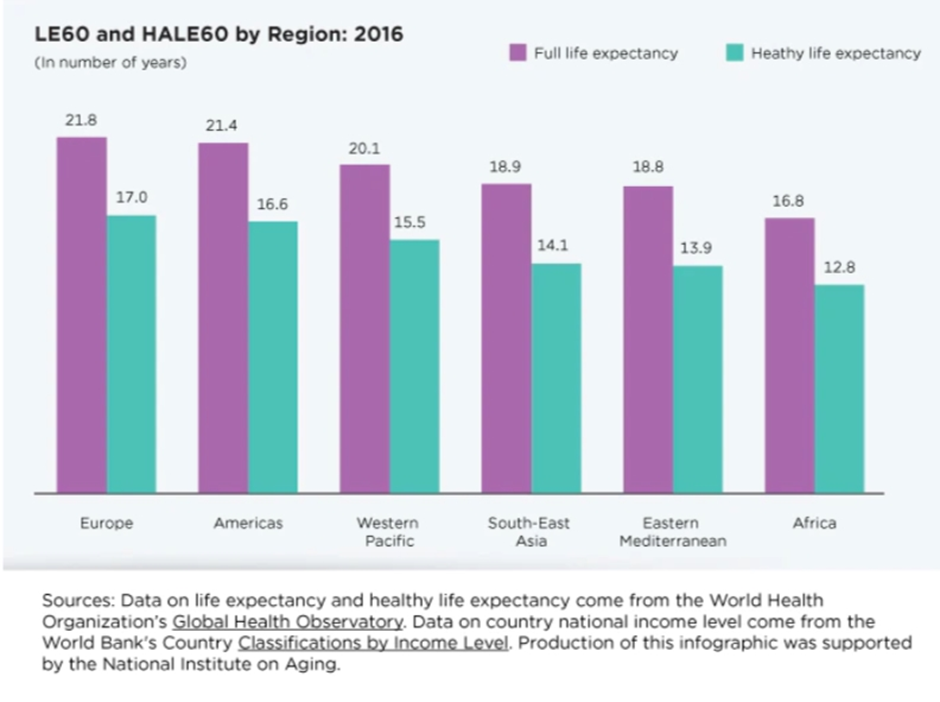
The projected number of years of good living after 60, or healthy life expectancy at 60 (HALE60), provides important insight into the prospective quality of life for older persons.
Healthy Life Expectancy at Age 60: 2000 to 2016 is a new Census Bureau infographic that depicts life expectancy and healthy life expectancy for persons over the age of 60.
According to Geographical Health Organization (WHO) data on Life expectancy and Healthy life expectancy, HALE60 was around a quarter shorter than LE60 in all world regions (7).
According to the report, health disparities are still a serious issue. “The average life expectancy disparity between low- and high-income countries is 18 years, while the gap between the lowest and highest life expectancy is 30 years,” it says.
Low-income countries have maternal mortality rates that are up to 100 times greater than high-income countries. While 80 percent of children with cancer survive in rich countries, and just 30 percent of children with cancer survive in low-income countries (4).
As regional trends are significant, differences in factors such as economic levels, national health legislation, and cultural norms can generate huge changes in life expectancy and good life expectancy within an area (7).
How did the pandemic alter our perceptions?
People hospitalized with Covid-19 infection had significantly higher levels of oxidative stress, dramatically lower levels of glutathione, one of the most abundant physiological antioxidant, according to US researchers (8).
Oxidative stress is caused by an accumulation of free radicals, highly reactive molecules that can destroy cells, membranes, lipids, proteins, and DNA. Cells in the body create glutathione to protect themselves from oxidative damage. Cells that are unable to neutralize free radicals can cause cellular damage, which can impact a wide range of physiological functions.
Infection with COVID-19 causes an overactivation of monocytes/macrophages, resulting in a cytokine storm and, as a result, the onset of acute respiratory distress syndrome (ARDS) (9).
According to MHI, we need to profoundly redefine what it means to be healthy. Individual ambitions and scientific study no longer support the traditional concept of good health as just the absence of illness.

Fig 1: COVID-19, and the social determinants of health
According to the research, we should return to a 70-year-old concept. The founding constitution of the World Health Organization defined health as “a condition of total mental, physical, and social wellbeing, not only the absence of disease or disability” in the earlies 1948. This definition, according to McKinsey, “recognizes the significance and interdependencies of mental, physical, social, and spiritual components,” and should be the foundation of a novel strategy to better living (4).
Steps to a healthier and fulfilling life
The document proposes stages that would result in an incremental 45 billion years of higher-quality human life over the world(4). These are the following:
- Put a greater emphasis on preventing and fostering healthy behavior.
According to the analysis, the economic advantages of increasing global population health would be up to four times the costs involved. Only 2.8% of OECD countries’ health spending are spent on preventative measures, immunization, and health education.
- Strong data will aid in health assessment and comprehension.
“Measurement is crucial to improvement.” It can assist in determining what works and directing resource allocation. Only 5% of the components that influence a holistic picture of health are carefully measured.
- Develop a sense of common purpose
Although no single player can address the core causes of disease, many players do not appear to be attempting to do so. In PwC’s 2019 HRI global consumer survey, 57% of respondents claimed that they had not explored socioeconomic variables with their doctor. It will take a coalition of partners from both inside and beyond the healthcare industry, with leaders finding ways to genuinely connect their aims.
- Generate data insights to aid in decision-making
The Visiting Nurse Association of Texas’s Meals on Wheels program used predictive analytics to build a virtual population and demonstrate how different treatments affected their health. According to the research, nutritious meal delivery minimized chronic illnesses, conserving the community an average $10.4 million in annual health costs and preventing 24 heart attacks. There were 12 fewer hospitalizations for congestive heart failure and 12 fewer strokes. This strategy may be used to mimic a variety of interventions, from the creation of new walking pathways to the provision of emotional support to socially isolated people.
- More and faster innovation is required.
Prior to COVID-19, the previous best to manufacture a vaccine was four years. Vaccines for COVID were made available in under 12 months, demonstrating the possibility of rapid innovation. During the epidemic, investment in digital health tools more than doubled.
- Empower people to take charge of their own health.
According to the report, low activity levels, unhealthy diets, lack of sleep, pharmaceutical use, and smoking are responsible for up to 60% of fatalities worldwide. Social media could be used to persuade people to change their harmful habits.
A substantial improvement in health would “demand unprecedented teamwork to transform society’s ideas and actions enough to realize possible increases in life expectancy and quality of life”.
The time has come!
Governments, payers, hospitals, pharmaceutical firms, community groups, tech businesses, and new entrants all have something to lose. We will be unable to afford the unsustainable expenditures caused by rising rates of disease unless we take strong steps. We can identify the conveners who bring people together while collecting and analyzing data that can reveal key areas where we can act with support to assist individuals in making better choices.
References:
- Stephen Jivraj, Alissa Goodman, Benedetta Pongiglione & George B. Ploubidis (2020): Living longer but not necessarily healthier: The joint progress of health and mortality in the working-age population of England, Population Studies
- Mackenbach, J. P., and C. W. N. Looman. 2013. Life expectancy and national income in Europe, 1900–2008: An update of Preston’s analysis, International Journal of Epidemiology 42(4): 1100–1110.
- Kontis, V., J. E. Bennett, C. D. Mathers, G. Li, K. Foreman, and M. Ezzati. 2017. Future life expectancy in 35 indus[1]trialised countries: Projections with a Bayesian model ensemble, The Lancet 389(10076): 1323–1335.
- https://www.weforum.org/agenda/2022/04/longer-healthier-lives-everyone/
- Jivraj, S. 2020. Are self-reported health inequalities widen[1]ing by income? An analysis of British pseudo birth cohorts born, 1920–1970, Journal of Epidemiology and Community Health 74(3): 255–259
- Ploubidis, G. B., A. Sullivan, M. Brown, and A. Goodman. 2017. Psychological distress in mid-life: evidence from the 1958 and 1970 British birth cohorts, Psychological Medicine 47(2): 291–303.
- https://www.census.gov/library/stories/2021/05/long-life-does-not-always-mean-a-healthy-life-in-old-age.html
- Derouiche S (2020) Oxidative Stress Associated with SARS-Cov-2 (COVID-19) Increases the Severity of the Lung Disease – A Systematic Review. J Infect Dis Epidemiol 6:121.
- Prompetchara E, Ketloy C, Palaga T (2020) Immune responses in COVID-19 and potential vaccines: Lessons learned from SARS and MERS epidemic. Asian Pac J Allergy Immunol 38: 1-9.